The relevance of grade in follicular lymphoma
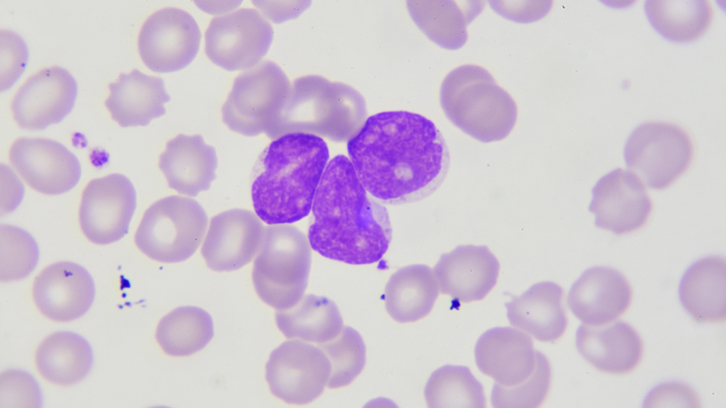
Follicular lymphoma (FL) is the most common type of indolent (i.e., generally slow-growing) lymphoma. It is a clonal proliferation of germinal center B-cells, initiated (in a large majority of cases) by a translocation between chromosomes 14 and 18, t(14;18), which gives rise to the fusion gene IGH-BCL2. This translocation causes an increase in expression of protein bcl2 which leads to cellular resistance to apoptosis (programmed cell death). The typical malignant cells (centrocytes) are small, as opposed to centroblasts, cells characterized by their large size and immature appearance, two features generally associated with aggressiveness in lymphoid malignancies. The world health organization (WHO) recommends grading FL according to the number of centroblasts per high-power field; cases with fewer than 6 per field are classified as grade 1 FL while those with > 15 are grade 3 (grade 2 being those with 5 to 15 centroblasts). Grade 3 is further divided into grade 3A (FL3A) when centrocytes are still present and grade 3B (FL3B) when they are absent (all cells being centroblasts).
Although there are historical reasons behind grading (different grades could be classified as different disorders before the WHO classification), currently there is also a scientific purpose. Low grade FL (grades 1 and 2), the most common, has a high prevalence of t(14;18) and is often CD10-positive (a marker of germinal center origin). These two elements are important (although not required) for the diagnosis of FL. Conversely, both are less frequent in FL3B. Furthermore, unlike low grade FL, FL3B frequently coexists (i.e., is commonly found in the same lymph node) with diffuse large B-cell lymphoma (DLBCL, an aggressive lymphoma). It is, therefore, conceivable that there is a biological continuum between low grade FL and some types of DLBCL, with grade 3 FL somewhere in between. Unfortunately, the available evidence only partially supports this hypothesis and the relationship between the different grades of FL and DLBCL remains unclear.
With this uncertainty come unresolved practical questions, which we posed in a recent letter to the editor of Annals of Oncology. Since DLBCL is curable, unlike FL (generally), it is of utmost interest to determine whether FL3 is curable. Although the consensus is that FL3 (or, at least, FL3B) is probably curable, large studies have not offered conclusive results. This is due to a variety of causes (particularly the rarity of pure FL3, without the coexistence of either low grade FL or DLBCL, the different treatment regimens employed, and the lack of agreement between pathologists in diagnosing FL3) which have prevented obtaining a large and homogenous enough series of cases to determine the natural history of FL3. The second concern is that, under the notion that FL3 (or, at least, 3B) is curable, they are often treated as DLBCL, with the chemotherapy regimen RCHOP, which is also one of the front line alternatives for FL. However, it is likely that the first choice for DLBCL changes in the next few years, at least for some subtypes. If this was the case, consensus-based treatment of FL3 as DLBCL would no longer be a valid option, and solid evidence for the best treatment of FL3 will be required.
ICO-Hospital Germans Trias i Pujol
Institut de Recerca Josep Carreras
Universitat Autònoma de Barcelona
References
M. Sorigue, J. M. Ribera, J.M. Sancho The clinical dilema of grade 3 follicular lymphoma. Annals of Oncology, Volume 27, Issue 10, 1 October 2016, Pages 1974. https://doi.org/10.1093/annonc/mdw284

